Tooth fractures are more commonplace than you would think. Teeth can crack, chip, or break for a multitude of reasons, creating intense pain and potentially harmful complications. Fortunately, having your dentist assess the problem and provide treatment strategies will help you avoid excessive pain and irreversible damage.
Read on to discover the four most significant facts regarding tooth fractures, including symptoms, causes, and potential treatments.
1. How do tooth fractures look and feel?
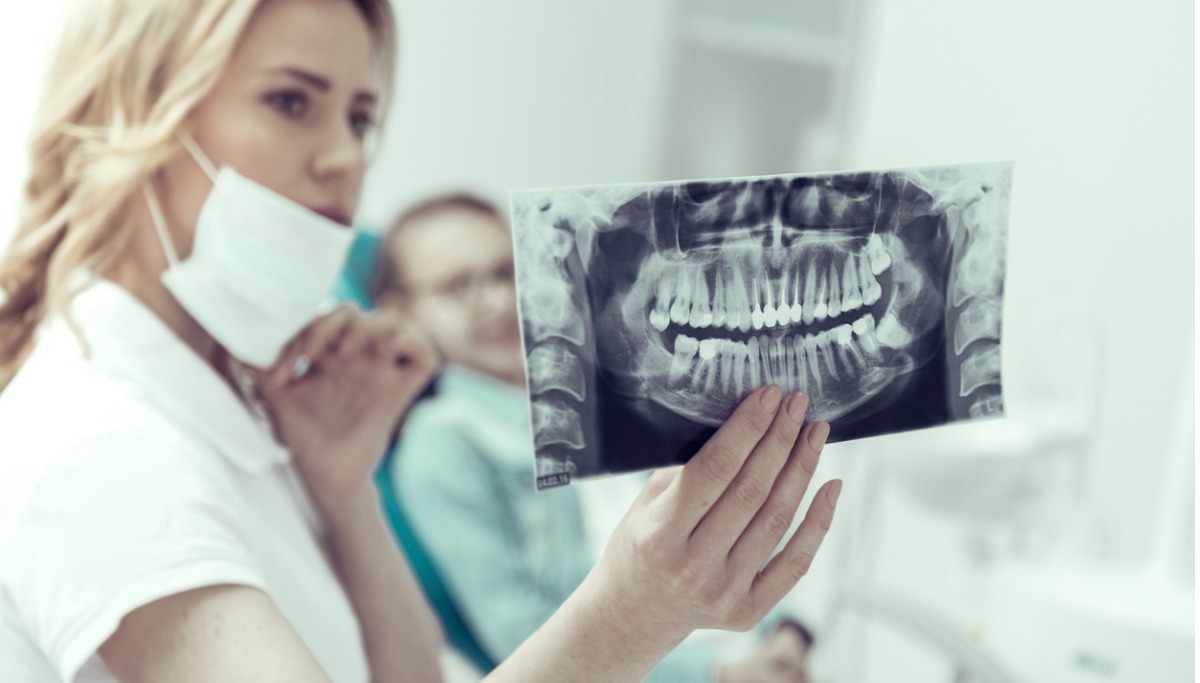
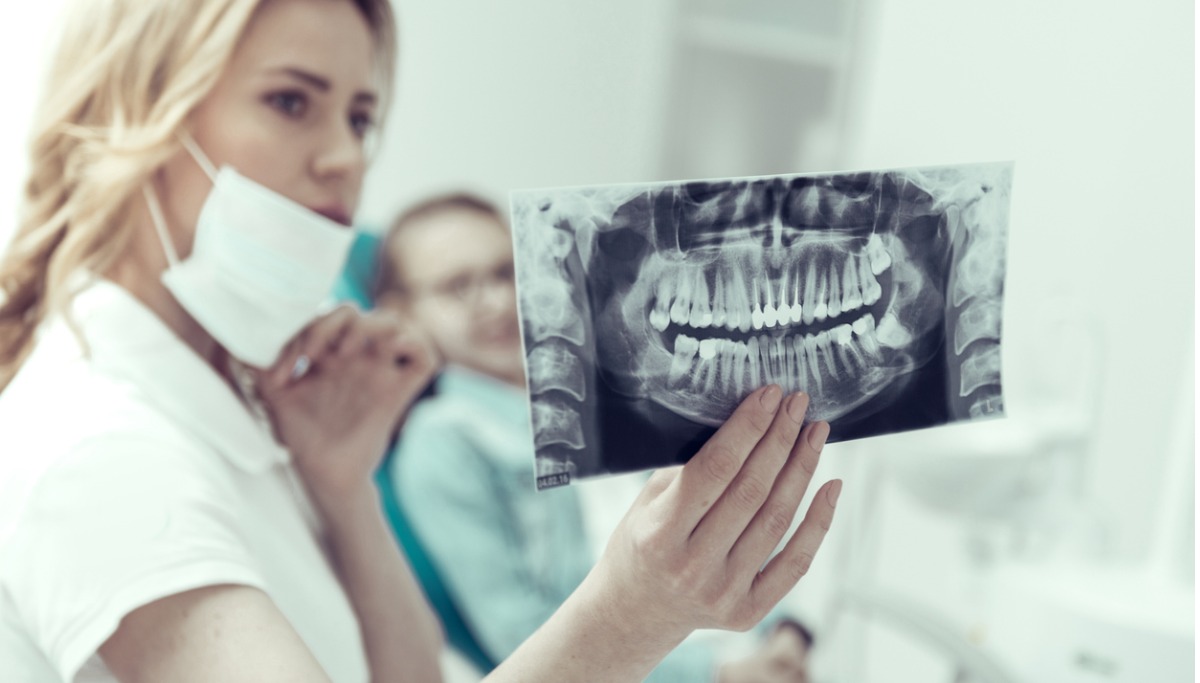
Tooth fractures are usually neglected for an extended period of time. They begin as microscopic splits on the typically smooth tooth surface, undetectable to the unaided eye. They can be spotted by your doctor by putting detecting dyes on your teeth.
Some fractures can be visible, resulting in unsightly chips and cracks. In severe cases, one or more of your teeth may break, leaving only the pulp and a fragment of dentin adhering to your jawbone.
Minor cracks in the outer surface of your teeth (also known as hairline cracks) can form without any symptoms. On the other hand, a significant break that causes tooth fragments to shift may irritate the pulp’s sensitive nerves, triggering excruciating aches when you eat, speak, or inhale air through your mouth. Furthermore, the untreated pulp may be extremely sensitive to hot and cold foods and beverages.
2. Why do tooth fractures occur?
Enamel, your body’s toughest component, can only absorb so much damage. Biting down on a hard object with force can easily result in cracked or damaged enamel. Teeth can break and chip as a result of a blow to the face or jaw. Even natural wear and tear can be detrimental, especially in people over the age of 50 or who have bruxism.
3. How do tooth fractures trigger other problems?
Tooth fractures not only inflict agonizing tooth pain but also raise your chances of developing an infection in your mouth. Bacteria can infiltrate the inside of your tooth through even the smallest holes and cracks in the enamel. Infection, excruciating jaw pain, and toothache are all potential outcomes.
An oral infection should not be underestimated. If left untreated, it can have severely dangerous consequences. Bacteria can affect the roots of neighboring teeth or spread to the rest of your body through blood vessels in your jaw, increasing your risk of potentially deadly diseases. To avoid this, it is recommended to seek medical help as soon as possible.
4. What are the restorative options?
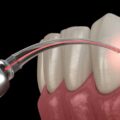
The degree of the fracture and the injured area of the mouth determine the treatment for tooth fractures. If there are only a couple of minor cracks, ongoing monitoring for changes may be necessary. Restorative therapy may be required if the damaged tooth is extremely sensitive or has been infected with bacteria, resulting in further damage.
Consider dental veneers to prevent and conceal front-tooth chips and fissures. This restorative treatment is both safe and inexpensive. A dental crown may be a better alternative if the affected tooth is weak or has had a root canal.
5. When must a tooth be removed and replaced?
A broken tooth may not always be saved by restorative treatment. Crowning the injured tooth cannot always repair a deep split or crack. Your tooth may be irreparably damaged, making it incapable of supporting the crown.
If this is the case, your dentist may advise you to have it extracted. Pulling the injured tooth both minimizes the chance of severe infection and relieves unbearable pain. Once the extraction site has healed, a dental implant can be used to replace the pulled tooth.































No Comments