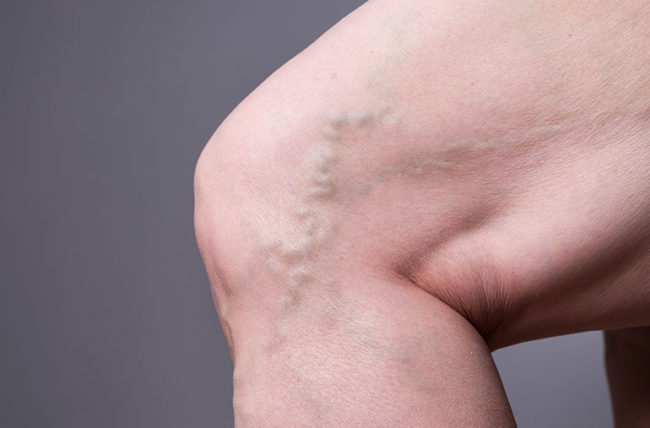
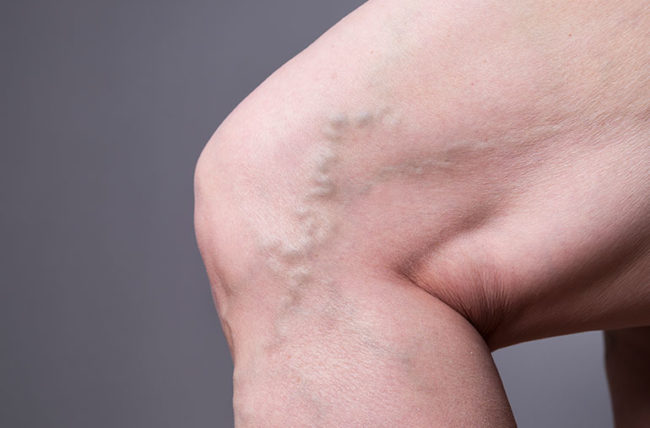
You may believe ropy, blue blood vessels in your legs are ugly but harmless. However, varicose veins can cause skin damage and potentially hazardous blood clots in certain people. Varicose veins are a common ailment. They affect almost one out of every four individuals in the United States, or about 22 million women and 11 million men between the ages of 40 and 80.
As they transport blood from your toes to your heart, your leg veins face an uphill battle. Small flaps, or valves, within these veins keep blood moving along this journey, and the pumping motion of your leg muscles aids in this process.
However, if these valves become weakened, blood might pool, increasing vein pressure. As a result of the increased pressure, your body tries to compensate by widening the veins, causing them to bulge and thicken, giving varicose veins their typical twisted look.
Despite the frequency of varicose veins, this condition is surrounded by various myths. But it’s important to stop believing these myths to ensure the health of your veins.
1. Varicose veins are part of the natural aging process
Aging definitely worsens varicose veins, though not everyone gets them. It’s a degenerative process that gets worse and more prominent as we age. But young people can get varicose veins, too. While the average age of patients treating varicose veins is 52, this condition might affect patients as young as 13.
If you’ve got varicose veins, it may run in your family. The cause of varicose veins is primarily genetic. Changes in hormone levels also come into play as a risk factor for varicose veins. For this reason, your risk can be made worse, especially by pregnancy.
2. Running causes varicose veins
Exercise, including running, is generally beneficial to your veins and improves circulation. Walking or running causes the calf muscles to pump more blood back to the heart. Running doesn’t cause varicose veins, but there is controversy regarding whether or not it makes them worse. During exercise, compression stockings can help prevent blood from collecting in your legs.
3. Varicose veins are always visible
While the varicose veins you see are on the surface of your skin, they can also be found deeper in the body, where they are not visible. It is entirely dependent on the leg’s structure. You couldn’t see them if there’s a lot of fatty tissue between the muscle and the skin. Surface veins are sometimes only the tip of the iceberg, and there’s a lot going on under the skin surface.
4. Varicose veins affect only women
While varicose veins are more common in women, men get them also. About one-quarter of adult women have some visible varicose veins, compared to 10 to 15 percent of men. However, the real number may be higher. The problem is that when men seek medical help, they’re often reluctant to ask about “minor” problems like varicose veins, spider veins, and leg swelling. Some even consider it “unmanly” to report varicose vein pain.
If you are a man with varicose veins, don’t hesitate to seek medical help for your problem. Varicose veins are a serious health problem that can lead to life-threatening consequences.
5. Surgery is the only treatment option
Stripping surgery, in which the vein is surgically removed from the body, is the only therapeutic option for varicose veins. That isn’t the case now. While this is still the most common varicose vein treatment in the world, less invasive techniques that leave no scars have grown in popularity in the United States.
Endothermal ablation, for example, entails delivering heat to a vein using a needle, forcing it to shut and stop to function. While the operation doesn’t leave a scar, it is uncomfortable, and you may need to be sedated before treatment. You may need to take a day off from work as well as a few days off from work to recover.
Some drugs, known as sclerosing agents, irritate a vein and cause it to shut. Others are adhesives that seal a vein shut without the need to numb the region. Although most therapies for varicose veins necessitate the removal of veins, your body has plenty of others that can take up the slack. You may consult a vein doctor to choose the procedure that will work best for you.


























![L1603_DogsBedTSk-86536723[1]](https://www.vipspatel.com/wp-content/uploads/2020/09/L1603_DogsBedTSk-865367231-120x120.jpg)







No Comments